Vaccination remained to provide the or same roughly the similar amount of prevention from hospitalization for persons up to the age of 75, according to the same statistics, and the doses remained 94 percent efficient amongst individuals aged 18-49.
COVID-19 vaccinations’ capacity to prevent people over 75 from hospitalization seems to be waning with time, but they were still 80 percent efficient as of the close of July, according to proposed federal statistics.
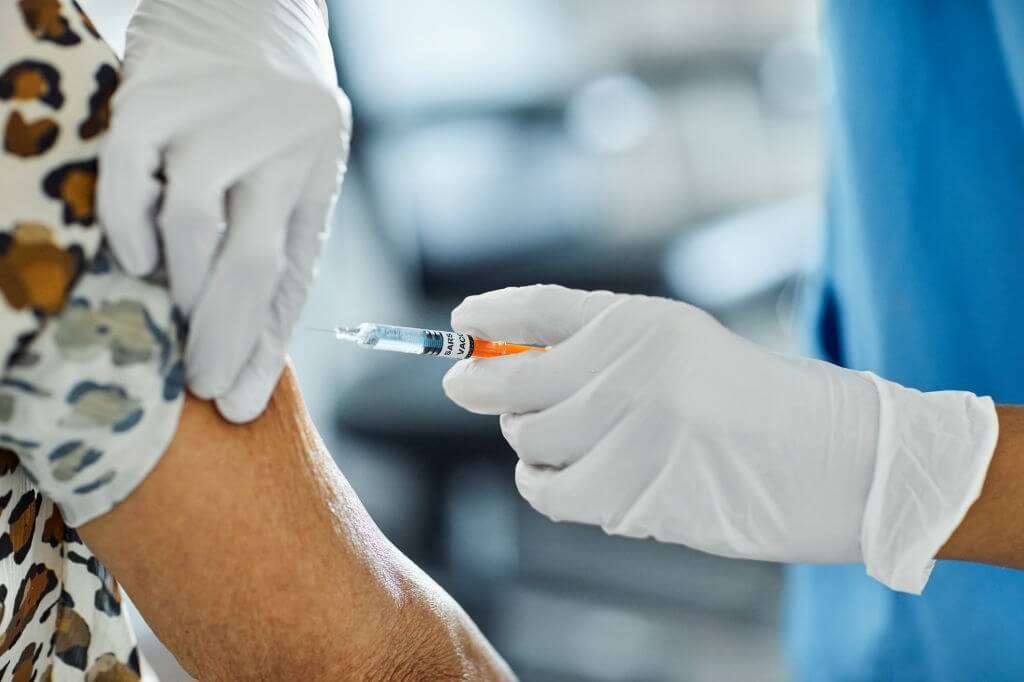
The Efficacy Of COVID Vaccines In Older Adults
Vaccination is still necessary: CDC Director Dr. Rochelle Walensky said earlier this month that “COVID-19-associated hospitalization rates were 17 times higher in unvaccinated”.
The new information was given at a meeting of the CDC’s impartial committee of vaccination specialists on Monday to review government preparations for a possible COVID-19 vaccination booster dosage next month.
As per statistics published by the US Centers for Disease Control and Prevention, hospitalization admissions amongst vaccinated adults were greater among elderly hospital patients and those with preexisting illnesses including such compromised immunological systems.
Older adults are people who suffer from various health issues and got low immunity. This makes them more prone to get infected and hence it is much needed to check the efficacy in this age group of people so that some better solutions can be provided to them.
They may get infected easily as they struggle regularly with BP, sugar, and many more diseases which make them compromise the immunity level, and even after doses of vaccines they may not have the desired level of an antibody that can counter the virus infection.
“It actually may be very difficult for us to disentangle time, since vaccination and the impact of the Delta variant, especially in some populations that we know were vaccinated earlier in the time course. So, if we see waning in the last couple of months, it could be really difficult,” Dr. Sara Oliver, a leading CDC vaccine official, told the vaccine panel.
Despite the fact only 16.1 percent of hospitalized COVID-19 individuals in June were completely immunized, the vaccinations proved to be “highly effective in preventing hospitalization,” according to a CDC analysis released over the weekend.
The CDC announced on Monday that a session of the group will be conducted in mid-September to evaluate further data on booster injections, possibly during the Biden administration’s scheduled roll-out of boosters injections the week of September 20.
Whereas the data reveal a minor drop in the vaccinations’ effectiveness to prevent elderly and fragile individuals from serious illness, the CDC says determining when much coverage seems to last in such populations is difficult.
Top US health authorities previously stated that 3rd dosage of the Pfizer and Moderna flu shots would’ve been needed 8 months since the first 2 shots, but fresh information from the flu shot manufacturers and other nations suggests booster shots may be needed way earlier than 6 months after immunization.
Nevertheless, older persons with co-morbidities or fragility have been mostly omitted, and no official statistics on safety and effectiveness in this population have been released. Even though the pandemic’s pace and impact on frail older individuals justify offering immunization to them first, individuals, their caregivers, and supervisory health care professionals will all have to make a decision on vaccination based on insufficient information.
The main applicant treatments that become available are reviewed here, with a concentrate on proof of safety and effectiveness in older people.
Generally, the limited data of Phase II trials suggest that healthy older adults have fewer immune reactions and moderate to severe adverse effects than younger persons. Many Trials had undertaken a concerted effort to enroll seniors, and intermediate evaluations of the Pfizer &Moderna vaccines have resulted in press releases claiming great efficacy.