The peer-reviewed article, which was released today in Clinical Statistics, employs a new method to indicate that laterally flowing testing (LFTs) were likely greater over 80 percent efficient at identifying all degrees of COVID-19 disease and greater than 90 percent effective at finding highly contagious people.
This degree of precision is far greater than most prior research has revealed, and the scientists claim that the assays were a reliable security strategy for preventing disease transmission.
COVID-19 Transmission Risk Is Detected By Lateral Flow Testing
LFTs operate in a unique manner than polymerase chains reaction (PCR) assays, according to the scientists, and they cannot be matched “like for like.”
The effects of corona infection are primarily on the lungs, which gradually leads to other areas, and over a period, one has to succumb to death also. There are different tests conducted by experts to know the level of infection that one can spread to others, including various surfaces.
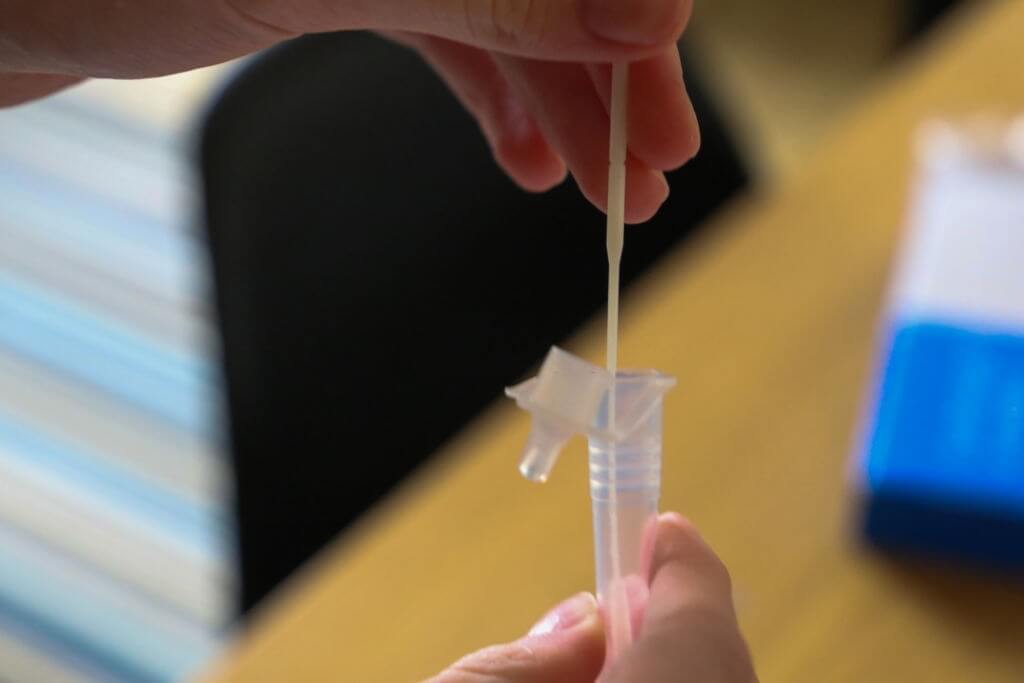
This test is known as LFT or lateral flow testing, from which it can be known how many people or places can be affected by an infected person. This leads to countermeasures of effective control on virus transmission to other people and areas.
PCR assays identify the virus’ genetic information, which could be around for weeks when an individual is no longer infected, but LFTs identify content from the virus’ outer protein thus were extremely certain to yield a good response while somebody is contagious.
“Previous studies comparing the reliability of lateral flow tests and PCR tests could be potentially misleading because a PCR test is a marker of having been infected at some point within a certain window of time and does not necessarily mean someone is infectious when testing positive,” said lead author Professor Irene Petersen.
According to a new publication produced by UCL researchers, “lateral flow tests are more accurate than previously reported and cannot be directly compared to how PCR tests function.”
“In most validation studies, individuals were tested simultaneously with LFTs and PCR tests, with PCRs being used as a gold standard to say someone is ‘positive or negative.’ The sensitivity of the LFTs was therefore evaluated by their ability to identify the same cases that the PCRs picked up. However, this is like comparing apples and oranges.”
The publication includes a method for measuring the sensitivities of LFTs as well as an instance of a Liverpool investigation. A head-to-head verification in the Liverpool trial found that LFT’s responsiveness is just 40%.
Nevertheless, the UCL-led study estimates that, in actuality, the responsiveness of the usual Liver Function Tests in identifying somebody who is probably to be contagious is over 80 percent, following accounting for the variations among both the testing with the genetics of COVID-19.
Professor Michael Mina said: “There is a spectrum of infectious amounts of the COVID-19 virus and we show that LFTs are likely to detect cases 90–95% of the time when people are at their most infectious. The tests could achieve even 100% sensitivity when viral loads are at their peak and therefore catch nearly everyone who is currently a serious risk to public health”.
Professor Petersen added: “As LFTs are becoming widely used in schools, workplaces, and for admittance to venues such as those used for large events, it is important that health professionals and the public have clear information about the operating characteristics of the tests. We have demonstrated that the absolute sensitivity to detect SARS-CoV-2 antigens is likely high with LFTs”.
The researchers recognize that the sensitivities of the LFTs are, of necessity, affected by sample mistakes and the expertise of the individual conducting the sample and testing, so much uncertainty was not factored into their equation adjustments.